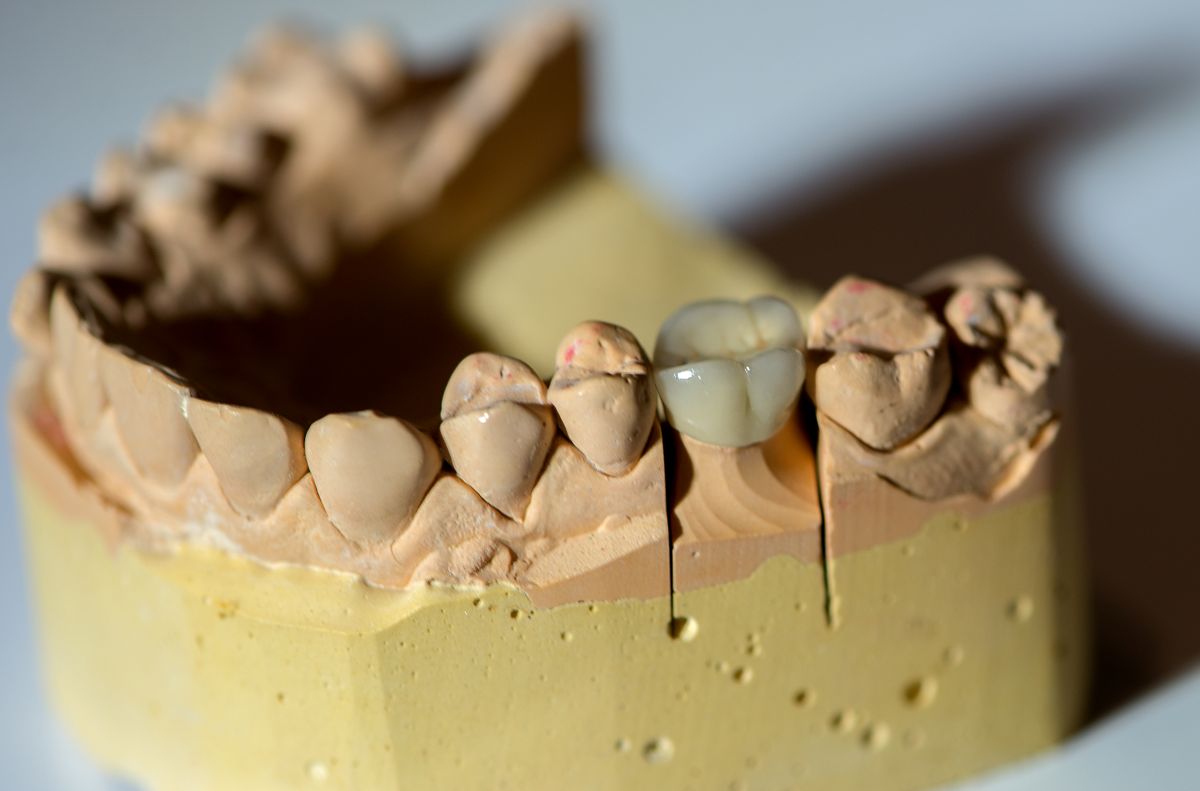
A dental crown is one of the most reliable ways to restore a tooth that has been weakened by decay, fracture, or a large existing restoration. It is also one of the most commonly delayed treatments in dentistry. Patients manage symptoms, work around a sensitive tooth, or skip a follow-up after a root canal because the pain resolved. By the time they come in, the situation has often become more complicated than it needed to be.
Understanding when a crown is the right call makes it easier to act at the point when the outcome is best. Here are seven signs that a tooth may need one.
1. Pain when biting or chewing
Pain that appears specifically when biting down, particularly on one side, is one of the most consistent indicators of a tooth under structural stress. It often points to a crack that does not show on an X-ray, a fractured cusp, or a large filling that is no longer holding the tooth together the way it once did.
This kind of pain is easy to dismiss because it is inconsistent. It may flare on something hard and then disappear for days. That pattern does not mean the tooth is fine. It usually means the problem is positional, loading only under specific bite angles.
A tooth that has been structurally compromised in this way will eventually fracture completely if left without treatment. At that point, a crown is often no longer an option. For patients who carry jaw tension or grind at night, the risk is compounded. TMJ and bite balance are an important part of how Dr. Wolfe plans any crown restoration.
2. A cracked or fractured tooth
Teeth crack from a single event, like biting down on something hard, or from cumulative stress, like the slow weakening that happens around a large old filling. Some cracks are visible during an exam. Many are not.
When a crack reaches the dentin or pulp, it typically causes sensitivity to temperature, soreness with chewing, or an intermittent sharp sensation. If the crack extends below the gum line, additional treatment may be needed before a crown can be placed, and the prognosis becomes more uncertain the longer it is left.
A crown is the standard treatment for a cracked tooth because it wraps the entire tooth and distributes bite forces evenly across the surface, rather than allowing pressure to concentrate at the crack site. A filling addresses a void. It does not hold a cracked tooth together.
3. Decay that has taken too much tooth structure for a filling
When decay is caught early, a filling is the appropriate restoration. When a cavity has grown large, whether from time, a failed previous filling, or rapid progression, a filling may not be sufficient.
The clinical threshold is roughly half the tooth’s natural structure. When decay has compromised that much, a filling does not have enough sound tooth to bond to, and the remaining walls are at significant risk of fracturing under normal bite forces. A crown placed at this stage both restores the missing structure and protects what remains.
If a filling is placed when this threshold has already been crossed, the risk is not just that the filling will fail. It is that the tooth itself may fracture in a way that makes any future restoration much more difficult.
4. A tooth that has had a root canal
A root canal clears infection from inside the tooth and is often the treatment that saves a tooth from extraction. As a consequence of the procedure, the tooth loses the internal moisture that kept it flexible, becoming more brittle and more vulnerable to fracture under normal function.
This is why a crown after root canal treatment is almost always the recommended next step. Research consistently shows that root canal-treated teeth without crowns have significantly higher fracture and failure rates than those that are crowned. The crown is not a separate or optional treatment. It is the completion of the restoration.
Patients often delay or skip the crown after a root canal because the tooth no longer hurts. The absence of pain is not a sign the tooth is protected. The nerve has been removed. The structural risk remains, and it grows with every month the tooth is left uncrowned. Learn more about how dental crowns are planned at Encino Gentle Dental.
5. A large or failing old filling
Fillings have a lifespan. Over time, the bond between a filling and the surrounding tooth weakens. Small gaps open up at the margins. Bacteria can work their way underneath, causing new decay. The filling itself may crack or wear down, leaving the tooth underneath exposed.
When a large filling is failing in a tooth that has already lost significant structure, the problem compounds. The original cavity removed tooth structure. The failing filling has been the only thing holding the remaining walls together. Those walls are often thin.
At this stage, a crown is the appropriate next step. It covers the entire tooth rather than patching individual sections that are breaking down one by one. It also protects the tooth from the kind of fracture that can make a future crown impossible to place.
6. A severely discolored or misshapen tooth
Not every crown is placed for structural reasons. Some teeth are discolored in ways that do not respond to whitening, due to internal staining from old metal restorations, a history of trauma, or the effects of certain medications taken during tooth development. Others are misshapen in ways that affect both appearance and how the tooth functions within the bite.
For these teeth, an all-ceramic crown addresses both concerns at once. It covers the tooth entirely, corrects the discoloration or shape, and provides structural reinforcement. For patients planning a broader cosmetic treatment, a crown on a structurally compromised tooth often makes more clinical sense than a veneer, since a veneer covers only the front surface and depends on the underlying tooth being sound. Dr. Wolfe coordinates restorative and cosmetic planning together — visit the cosmetic dentistry overview to see how those decisions are made.
7. A tooth that is part of a bridge or implant restoration
Crowns are a core component of restorations that involve more than a single tooth. When a bridge is used to replace a missing tooth, the teeth on either side of the gap are fitted with crowns that anchor the bridge in place. Those anchor teeth need to be healthy, structurally sound, and strong enough to carry the added load over time.
For patients who choose a dental implant, a ceramic crown is placed on top of the implant post once it has fully integrated with the jawbone. The crown is the visible, functional part of the implant: what the patient chews with and what others see. For patients with TMJ concerns or bite imbalances, how an implant crown is designed and seated matters to the health of the jaw, not just the appearance of the smile.
What to do if any of these apply
A tooth that could be saved with a crown today may not be saveable six months from now. That is not a reason for alarm, but it is a reason to have the tooth evaluated sooner rather than later.
At Encino Gentle Dental, Dr. Wolfe evaluates each tooth in the context of your overall bite, jaw health, and treatment goals. All-ceramic and tooth-colored materials are used for crowns, with every restoration planned around bite balance and biocompatibility. If a crown is the right recommendation, the reasoning will be explained clearly. If a more conservative option is appropriate, that is the recommendation that will be made. Read more about Dr. Wolfe’s approach to care or visit our adult dental care page to see the full range of restorative services offered.
Patients from Encino, Sherman Oaks, Studio City, Calabasas, Tarzana, and the surrounding San Fernando Valley are welcome. Same-week consultations are available for new patients. Contact us to schedule an evaluation with Dr. Wolfe.
Frequently asked questions
How do I know if I need a crown or just a filling?
The main factors are how much natural tooth structure remains and whether the tooth is at risk of fracturing. When decay or damage has compromised roughly half or more of the tooth, or when the tooth has cracked, a filling is typically not sufficient. Dr. Wolfe will evaluate the tooth and explain the clinical reasoning behind any recommendation made.
Is sensitivity after a crown normal?
Some sensitivity in the days following crown placement is normal and usually resolves within one to two weeks. Sensitivity that persists beyond that period, or significant pain when biting, is worth calling about. The bite may need a minor adjustment, or there may be something that warrants a closer look.
Do I need a crown after a root canal?
In most cases, yes. A root canal-treated tooth is structurally more brittle than an untreated tooth and is at meaningful risk of fracture without a crown to protect it. The exception is sometimes made for certain front teeth with minimal structural loss, evaluated on a case-by-case basis. Dr. Wolfe will give a clear recommendation based on what the tooth actually needs.
How long does a crown last?
With consistent home care and regular dental visits, ceramic crowns typically last 10 to 15 years or longer. Longevity depends on bite forces, home care habits, and whether a nightguard is appropriate. For patients who grind, a nightguard can significantly extend the life of a crown and protect the surrounding teeth as well.
What about dental anxiety?
Crown procedures are among the treatments that most commonly cause apprehension. Dr. Wolfe’s practice offers sedation and comfort support for patients who need it, and each step of the process is explained before it happens. If anxiety has been a reason for delaying care, that is something the practice is experienced in working with.
When is a crown no longer an option?
If a crack extends below the gum line, or if decay has destroyed too much of the root structure, a crown may no longer be viable and extraction may be the only remaining option. This is one of the primary reasons early evaluation matters. The sooner a compromised tooth is assessed, the more options are still available.